Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Case Report - Open Access, Volume 2
Rupture of right non-communicating horn of bicornuate uterus with twin pregnancy
Verma Ruchi1; Patel Shweta2; Mishra Neha1,3*; Gupta Veena4
1Assistant Professor, Department of Obstetrics & Gynaecology, Government Institute of Medical Sciences, Greater Noida, M.L.N Medical College, Allahabad, India.
2Assistant Professor, Department of Obstetrics & Gynaecology, M.L.N Medical College, Allahabad, India
3 Senior Resident, All India Institute of Medical Sciences, New Delhi, India
4 Professor, Department of Obstetrics & Gynaecology, M.L.N Medical College, Allahabad, India.
*Corresponding Author : Neha Mishra
Department of Obstetrics & Gynecology, Government
Institute of Medical Sciences, Greater Noida, India
Email: imneha2908@gmail.com
Received : Jan 08, 2021
Accepted : Jan 28, 2021
Published : Jan 29, 2021
Archived : www.jcimcr.org
Copyright : © Neha M (2021).
Abstract
The rupture of uterus in first and second trimester is very rare and mostly associated with uterine anomalies or cornual pregnancy. Bicornuate uterus (BU) is a uterine anomaly results from incomplete fusion of the two Mullerian ducts during embryogenesis. Here we are presenting a case of primigravida in the second trimester (20 weeks) as ruptured ectopic pregnancy in emergency. Laparotomy showed BU with twin pregnancy in the ruptured non communicating right horn. Right horn excision was done. This case highlights the twin pregnancy in non-communicating horn of uterus and its rupture in early pregnancy. Cases with non-communicating horn are reported but twin pregnancy in noncommunicating horn is a rare one. In asymptomatic women, the presence of bicornuate uterus may not be detected until during pregnancy or delivery. In case of pregnancy in rudimentary horn, early sonographic diagnosis has a major contribution in evaluation and management. Treatment usually involved is resection of the ruptured horn. Since the scar is present on the uterus, it is important to avoid pregnancy for at least 1 year.
Keywords: Bicornuate uterus, Rudimentary horn, Twin pregnancy, Uterine rupture.
Citation: Ruchi V, Shweta P, Neha M, Veena G. Rupture of right non-communicating horn of bicornuate uterus with twin pregnancy. J Clin Images Med Case Rep. 2021; 2(1): 1011.
Introduction
The rupture of uterus at early gestation, i.e. in first and second trimester is very rare and mostly associated with uterine anomalies or cornual pregnancy. The female reproductive organs develop from the fusion of the bilateral paramesonephric (Mullerian) ducts to form the uterus, cervix, and upper two-thirds of the vagina. Bicornuate uterus (BU) is a rare uterine anomaly which results from incomplete fusion of the two Müllerian ducts during embryogenesis. This leads to varying degrees of separation between two symmetrical uterine cavities ranging from partial separation to complete separation with/without communication between the two cavities [1,2]. Co-existence of genitourinary anomalies are very common [3]. Rupture of the gravid uterus is a rare obstetric catastrophe with high mortality and morbidity. It is more common in multigravida or in scarred uterus and usually occurs at labor [4]. BU is associated with adverse reproductive outcomes. It could lead to rupture uterus during the pregnancy in second trimester [4]. Pregnancy in non- communicating rudimentary horn of bicornuate uterus is a rare phenomenon and twin pregnancy in rudimentary horn is rarer. Here we report a rare case of primigravida with twin pregnancy in rudimentary horn of bicornuate uterus which ruptured in second trimester mimicking ruptured ectopic pregnancy.
Case presentation
A 25-year-old primigravida presented to the emergency department as a case of 5 month amenorrhea with severe pain in abdomen for 5 days and syncopal attack and bleeding per vaginum since 1 day. Ultrasound scan performed one day before admission showed ruptured right sided ectopic pregnancy with a large heterogenic area of approx 19 × 69 mm in right adenexa having gestational sac (46 mm) with fetus of about 37.6 mm corresponding to 14 w 5 d with no cardiac activity and hemoperitoneum. Renal malformations were not detected by the ultrasound scan. The patient was pale and irritable. On examination, her blood pressure was 100/60 mm of Hg, pulse was 130/minute feeble and respiratory rate 30/minute. On Abdominal examination, guarding was present along with tenderness all over abdomen. On per speculum examination blood mixed discharge was present. On per vaginal examination, cervical os was closed, uterus anteverted soft corresponding to 8 weeks size with fullness in right fornix. Her hemoglobin was 4.0 g/L, liver function test and renal function were within normal limits.
Blood transfusion and fluid resuscitation was started immediately and the patient underwent exploratory laparotomy under spinal anesthesia.
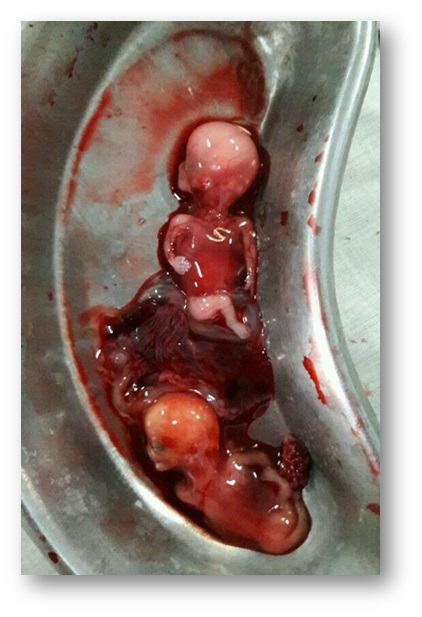
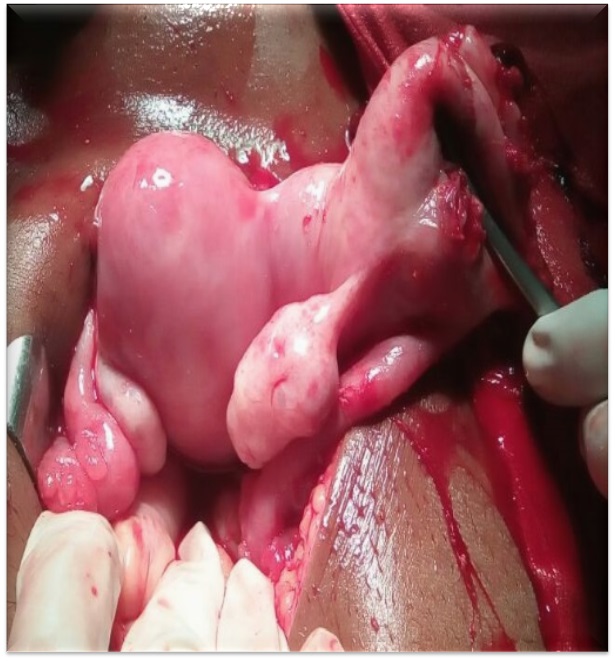
After taking full aseptic precautions abdomen was opened by sub-umbilical midline incision. 2.5 litres of hemoperitoneum was drained. Twin fetus corresponding 20 weeks of gestation were removed from peritoneal cavity. Uterus was found to be bicornuate. Left horn of the uterus, fallopian tube and ovary was apparently normal. Right horn of uterus was ruptured through 4 x 4 cm opening at fundus with bleeding from the edge. Right tube and ovary was normal. Resection of Ruptured right horn was done. The uterus was repaired in two layers with 1–0 vicryl. Patient stood the procedure well. Three units of packed red blood cells were transfused. Her post operative period was uneventful and stitches were removed on 8 day. She was advised to avoid conception for 1 year by using contraceptives.
Discussion
Pregnancy in a BU has a poor reproductive potential and requires close monitoring [1]. Normally it ends in the spontaneous rupture of rudimentary horn pregnancy with the clinical presentation of ectopic pregnancy. Our patient came in emergency with the history of 5 months amenorrhea with severe pain in abdomen and her ultrasound report showed finding of ruptured ectopic pregnancy. Our case is a rare entity because it had twin pregnancy in non-communicating rudimentary horn.
Casesof ruptured horn with singleton pregnancy has been reported by Mane and Kore et al. [4,5]. However, cases of twin pregnancy in noncommunicating horn has been reported very few in number. In asymptomatic women, the presence of bicornuate uterus may not be detected until during pregnancy or delivery [4,5]. Routine ultrasonography at 14–16 weeks in all antenatal clinics may help in early diagnosis, i.e., before rupture. This will decrease the mortality and morbidity associated with rapid and massive hemoperitoneum occurring because of rupture. Achiron et al. reported two cases of singleton pregnancy in rudimentary horn diagnosed by USG before rupture [6].
Treatment usually involved is resection of the ruptured horn. Since the scar is present on the uterus, it is important to avoid pregnancy for at least 1 year. If pregnancy occurs it is to be carefully monitored with early hospitalization and elective cesarean sections.
Conclusion
Pregnancy in non-communicating rudimentary horn of bicornuate uterus is a rare phenomenon but twin pregnancy in rudimentary horn is still rare. Therefore, high index of suspicion is warranted to detect this rare and very important complication of pregnancy before uterine rupture occurs.
References
- Singh N, Singh U, Verma ML. Ruptured bicornuate uterus mimicking ectopic pregnancy: A case report. J Obstet Gynaecol Res. 2013; 39(1): 364-6.
- Jayaprakash S, Muralidhar L, Sampathkumar G, Sexsena R. Rupture of bicornuate uterus. BMJ Case Rep. 2011; 28.
- Kochar S, Prakash P. An unusual case of rupture of right horn of bicornuate uterus at eighteen weeks of gestation. J Obstet Gynaecol India. 2012; 62(6): 694-5.
- Mane S, Choudhary R, Nandawar Y. An unusual presentation of pregnancy in bicornuate uterus. J Obstet Gynecol India. 1994; 44: 154–155.
- Kore S, Pandole A, Akolekar R, et al. Rupture of left horn of bicornuate uterus at twenty weeks of gestation. J Postgrad Med. 2000; 46: 39–40.
- Achiron R, Tadmor O, Kamar R, et al. Prerupture ultrasound diagnosis of interstitial and rudimentary uterine horn pregnancy in the second trimester: a report of two cases. J Reprod Med. 1992; 37: 89–92.