Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Case Report - Open Access, Volume 2
Foreign body in the scalp: A thorn in the flesh – case report
Kolawole Olubunmi OGUNDIPE1; Innih Asuekome KADIRI1; Taopheeq Bamidele RABIU2; Deborah Aanuoluwapo OLUWATUYI1
1 Plastic and Reconstructive Surgery Unit, Department of Surgery, Ekiti State University / Ekiti State University Teaching Hospital, AdoEkiti, Nigeria.
2 Neurosurgical Unit, Department of Surgery, Ekiti State University / Ekiti State University Teaching Hospital, Ado-Ekiti, Nigeria.
*Corresponding Author : Kolawole Ogundipe
Plastic and Reconstructive Surgery Unit, Department
of Surgery, Ekiti State University / Ekiti State University
Teaching Hospital, Ado-Ekiti, Nigeria.
Email: koogundipe@hotmail.com
Received : Feb 05, 2021
Accepted : Mar 12, 2021
Published : Mar 16, 2021
Archived : www.jcimcr.org
Copyright : © Ogundipe K (2021).
Abstract
Open scalp wounds are often associated with retained foreign bodies and are poorly reported. Despite meticulous radiological evaluations, foreign bodies can still be missed. Complication such as chronic headache, scalp abscess, chronic osteomyelitis, organic personality disorder had been reported. Coupled with the potential for medicolegal concerns, retained foreign bodied in the scalp thus require critical evaluation and management. Herein we reported a case of a retained stalk of grass (foreign body) in the scalp that is complicated with scalp abscess and chronic headache and call for a high index of suspicious in the management of foreign bodies in the scalp.
Keywords: Foreign body, Stalk of grass, Scalp injury, Scalp abscess.
Citation: Ogundipe K, Kadiri I, Rabiu T, Oluwatuyi D. Foreign body in the scalp: A thorn in the flesh – case report. J Clin Images Med Case Rep. 2021; 2(2): 1026.
Introduction
Scalp wounds are not uncommon in developing counties especially following trivial road traffic injuries [1]. Such open wounds are often complicated by the inclusion of foreign bodies. The tendency for foreign bodies not to be detected is high. This is particularly more likely in the scalp due to its high vascularity and potential for bleeding when injured. Imaging of lacerations has been advised to enhance the detection of foreign bodies, as they represent potential areas for medicolegal concerns [2]. However, in some cases the imaging may not reveal the foreign bodies, thus necessitating a re-exploration of the wound. Pending exploration, the presence of the foreign bodies may be complicated by recurrent infection, including chronic osteomyelitis.
Case report
Mr OA, a 45-year-old farmer was referred to the plastic surgery clinic on account recurrent discharge from a scalp wound of about 6 months duration.
He was well until about 8 months before presentation when he sustained a road traffic injury, including an injury to the scalp. There was no associated loss of consciousness, convulsion, vomiting or persistent headache. The scalp wound was sutured at a General Hospital and was said to have been dressed for about a month before it healed. The wound was however said to have been recurrently discharging pus since a month after.
He presented to the general outpatient department of our facility 5 months after the injury with a history of recurrent discharge and an assessment of poor wound healing secondary to the inclusion of a foreign body was made. CT scan requested for showed maxillary sinus polyp and scalp cellulitis. No foreign body was visualized. He was placed on antibiotics (Tabs Cefuroxime).
Two weeks later, he returned with complaints of headache which had persisted for a week. A skull X-ray was requested which was essentially normal. He was then referred to the plastic surgery unit for further management.
At the plastic surgery clinic, he was examined and found to have a sinus at the left parietal region not actively discharging and a firm, non-tender swelling measuring 4 cm X 4 cm at the ipsilateral parietal region posterior to the sinus. An assessment of recurrent scalp discharge secondary to likely chronic osteomyelitis of the skull bone, to rule out scalp abscess was made. He was continued on antibiotics and referred to the neurosurgery clinic.
The neurosurgeon assessed him as possibly having left parietal scalp abscess, skull osteomyelitis, or foreign body. It was also noted that the earlier CT scan done showed scalp collection with no bony involvement (although there was no bone window). A repeat CT scan with a bone window was requested which showed an area of hypodense swelling over the left parietal region with no involvement of the underlying bone and no evidence of intracranial extension. A well marginated hypodense lesion was also seen within the left maxillary sinus which is also in keeping with a polyp. An assessment of chronic left parietal scalp abscess was made, and he was once again referred to the plastic surgery unit for further review and continuation of care.
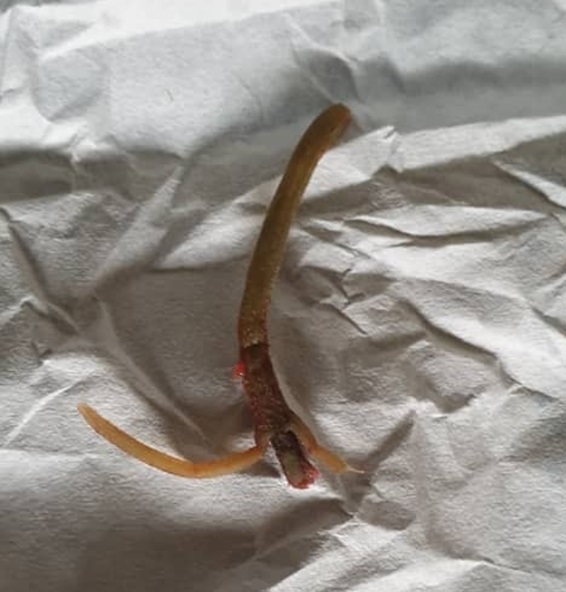
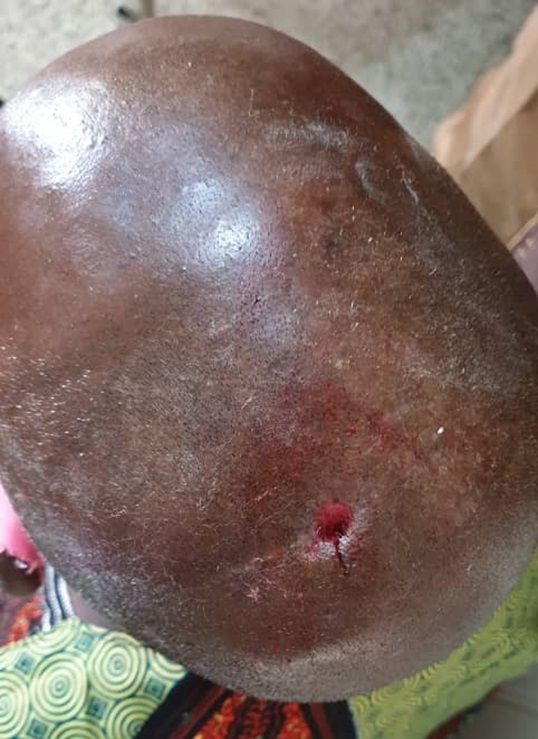
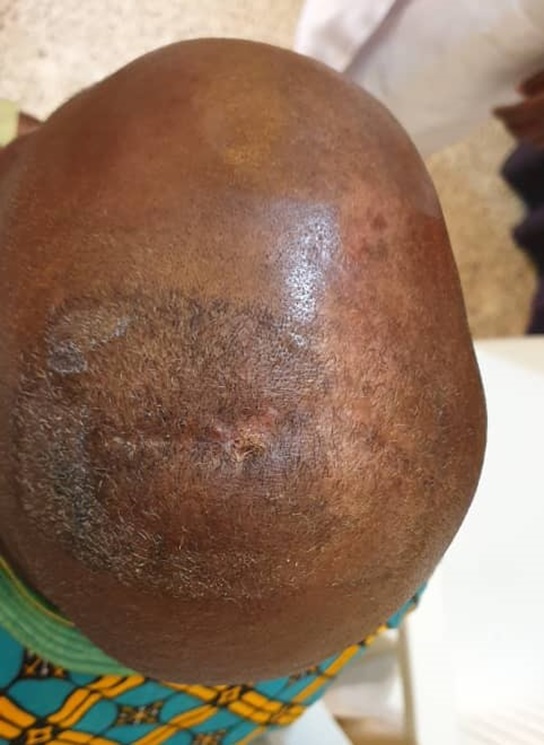
Exploration of scalp swelling was done in the Plastic surgery clinic under local anaesthesia and a foreign body (stalk of grass of 5 cm in length) was found and removed from the sub-galeal space, the cavity was curetted with forceps, cleaned out and wound dressed with honey (Figures 1 and 2). He was continued on antibiotics (Cefuroxime) and paracetamol and had alternate day wound dressing for about 2 weeks. Scalp wound has healed completely, and the patient’s condition is satisfactory (Figure 3).
Discussion
Model validation and test with unknown data
Scalp lacerations are different from lacerations in other parts of the body because of its unique anatomy and blood supply. Prime attention should be given to securing haemostasis and removal of foreign bodies, if present, in patients with scalp laceration [4]. The removal of the foreign bodies may however be a dilemma in the face of marked bleeding from the scalp following trauma.
Presence of foreign bodies in the scalp can present in diverse ways. A case of intracranial foreign body in a 9-year old boy presenting with recurrent headache [3]. Our patient had also complained of a persistent headache. In patients with a history of trauma, foreign body associated headache should always be suspected. Singh in 2007 [1] reported retained cotton gauze (foreign body) in the scalp that was associated with an organic personality disorder. Though our patient did not present with a classic organic personality disorder, the level of anxiety and depressive thoughts he demonstrated were significant. Local pain and swelling have also been associated with foreign bodies in the scalp. Patel [5] in a case contribution had reported a patient with an injury to the scalp in a road traffic injury who presented with 5-6 weeks history of local pain and swelling. Surgical exploration revealed a foreign body which turned out to be a thorn. The foreign body in our patient too turned out to be a fleshy thorn. He had parietal swelling with a recurrent discharge of 6 months duration. Because it was a thorn - a stalk of grass, radiological examinations (skull X-ray and CT scan) could not identify the foreign body. However, the CT scan showed a hypodense swelling over the left parietal region with no involvement of the underlying bone and no evidence of intracranial extension. In patients with such swelling suggestive of scalp abscess, who had prior histories of trauma, a high index of suspicion of foreign bodies should make wound exploration a must.
The importance of imaging of lacerations had been underscored by a couple of reports [2,6]. However, the Skull X-ray and CT Scan carried out by our patient did not reveal any foreign bodies as he presented with a non-lucent foreign body. As advised, standard evaluation of open scalp wound should include a thorough history, physical examination, a high index of suspicion of retained foreign body, wound exploration with irrigation, and at times wound debridement.
Wound exploration, which was done as a clinic procedure, revealed a fleshy thorn, a stalk of grass, which was extracted from the sub-galeal space. The sub-galeal space consists of loose areola tissue, it is not surprising therefore that the foreign body is lodged in the space. There is no reported case of such stalk of grass as a foreign body in the scalp. This, therefore, adds up to the body of literature. Following wound exploration, the patient wound healed fully within two weeks, thus ending an eight-month ordeal of morbidity. This reinforces the need to explore the scalp when retained foreign bodies are suspected.
Conclusion
Scalp wound following trivial injuries is common. Complications arising from retained foreign bodies may result in significant morbidity with attendant possible medicolegal concerns. This case should remind us of to have a high index of suspicion and be willing to explore whenever we are confronted with scalp injuries with potential for inclusion of foreign bodies.
References
- Singh GP. A rare case of head (scalp) trauma with foreign body. Indian Journal of Psychiatry. 2007; 49(4): 299.
- Fowler TR, Crellin SJ, Greenberg MR. Detecting foreign bodies in a head laceration. Case Reports in Emergency Medicine. 2015; 801676: 2.
- Isikay S. Foreign body in the scalp: A rare cause of recurrent headache. Indian J Paediatr. 2016; 83(8): 871–872.
- Almulhim AM, Madadin M. Scalp laceration. In: StatPearls. StatPearls Publishing, Treasure Island (FL). 2019.
- Patel MS (2016). Foreign body – scalp. Radiopaedia. Accessed at: https://radiopaedia.org/cases/foreign-body-scalp
- Patel PM, Blackburn TPD, Tait MJ, Strong AJ. Cranial blade: Retained for 3 years. British Journal of Neurosurgery. 2004: 18(1); 74-75.