Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Case Report - Open Access, Volume 2
Migratory non-itchy rash
Sami Hoshi
Division of Infectious Diseases, Department of Internal Medicine, Thomas Mackey Center for Infectious Disease Research, Ascension St. John Hospital, Detroit, MI, USA.
*Corresponding Author: Sami Hoshi
Division of Infectious Diseases, Department of
Internal Medicine, Thomas Mackey Center for Infectious Disease Research, Ascension St. John Hospital,
Detroit, MI, USA.
Email: sami.hoshi@ascension.org
Received : Apr 19, 2021
Accepted : Aug 20, 2021
Published : Aug 25, 2021
Archived : www.jcimcr.org
Copyright : © Hoshi S (2021).
Citation: Hoshi S. Migratory non-itchy rash. J Clin Images Med Case Rep. 2021; 2(4): 1282.
Short report
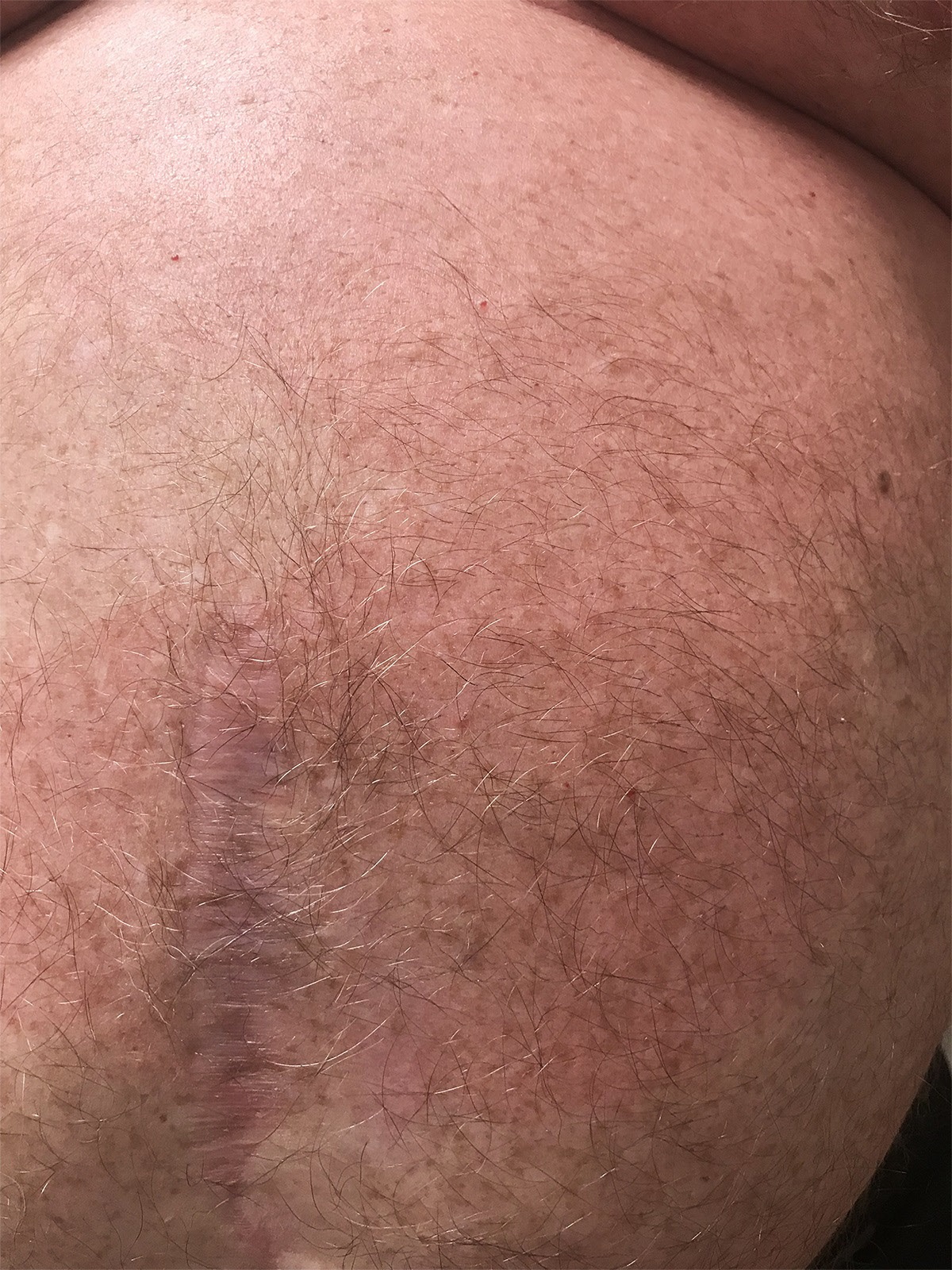
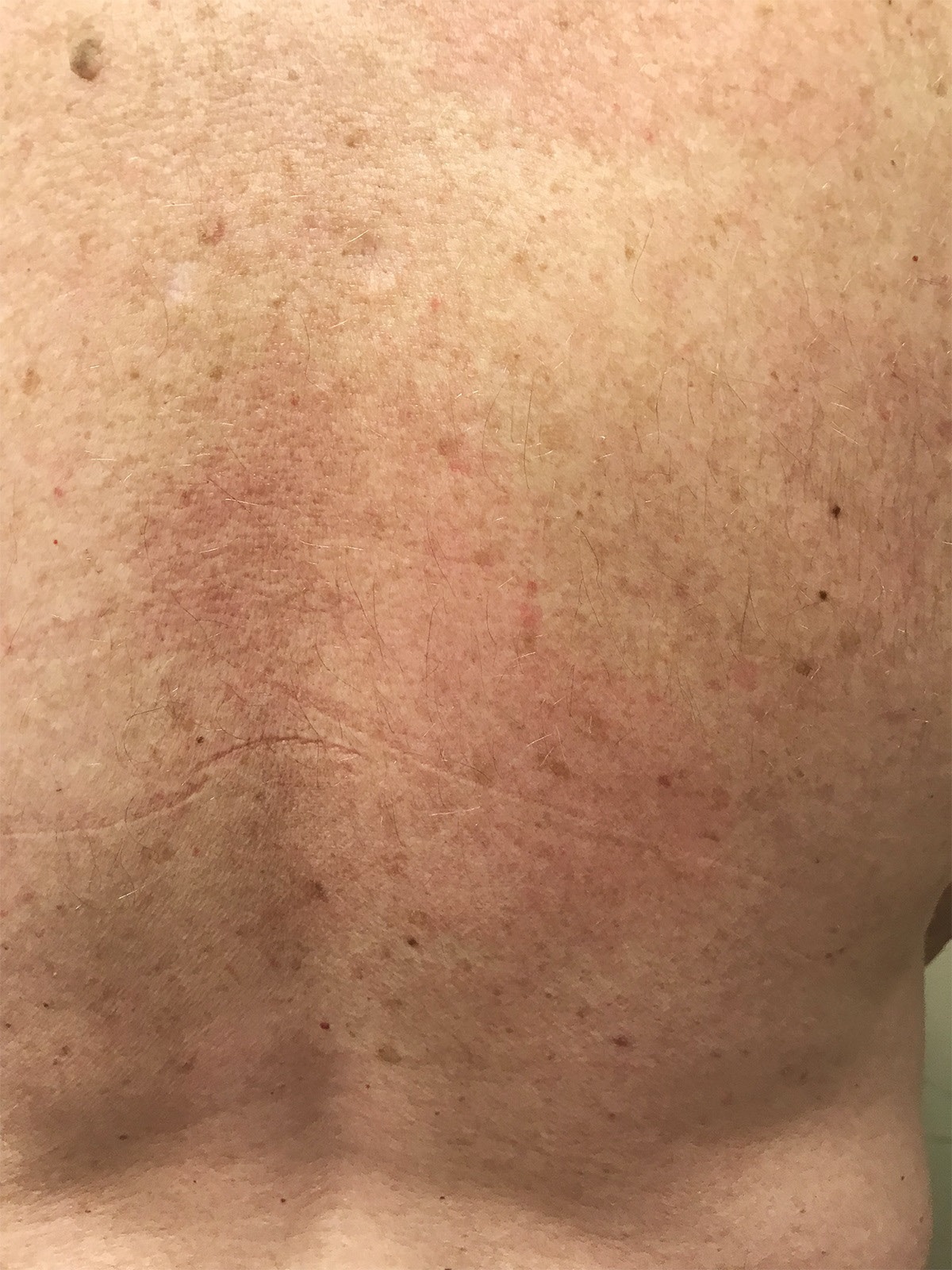
A 58-year-old man presented with 4-day history of multiple, erythematous, non-itchy, painless, patchy spots, along with fatigue and jaw pain. This rash started around the periumbilical area and then spread over his chest and right upper back (Figure 1,2). There was no involvement of face, mucous membranes, and extremities. He denied any sore throat, cough, or other symptoms. Besides the skin rash, his physical examination was unremarkable. There was no temporomandibular joint swelling, or joint tenderness. A month ago, he travelled along with the west coast of Michigan – a Lyme-endemic region of the USA and noted his exposure to mosquitoes. Shortly after his visit, he recalled having fever, chills, myalgia and a similar patchy groin rash which resolved in a few days. At that time, blood work by his family physician revealed mild transaminitis. At the current visit, repeat blood work and electrocardiogram were normal. A clinical diagnosis of early disseminated Lyme disease was made. Lyme Ab IgM and IgG were both elevated, as was his Western blot test. He was given a 10-day course of doxycycline. He reported complete resolution of his symptoms at follow up.
Lyme disease is caused by Borrelia burgdorferi, a spirochete transmitted by the Ixodes tick. These ticks are endemic to the Northeast, Midwest and Pacific Coast regions of the USA and most cases occur in individuals who live, or travel to these regions. At the site of tick bite, patients with early Lyme disease develop Erythema Migrans (EM) rash in 1-2 weeks (range, 3 to 32 days) [1]. EM is a uniform erythematous oval to circular rash that can form a zone of central clearing. In some patients, EM may be asymptomatic, but most patients may have nonspecific viral symptoms of fatigue, fever, chills, myalgia, headache and mild transaminitis. In the following weeks, spirochete disseminate hematogenously and patients can present with multiple erythematous rings with central clearing. Our patient presented in this stage of early disseminated Lyme disease. In addition, a patient may develop myalgia and arthralgias without arthritis, as in our patient who had transient jaw pain. Cardiac involvement with conduction blocks and neurologic complications with cranial nerve palsies, can occur at this stage. Migratory arthritis of large joints presents as late disseminated Lyme disease in addition to the cardiac and neurologic manifestations. Diagnosis can be made clinically on the cutaneous findings alone, or by serological testing. Standard 2-tiered testing involves enzymelinked immunoassay followed by Western blot. [2] Treatment depends on the symptoms present and the stage of disease. Early Lyme disease can be treated orally with doxycycline, cefuroxime and amoxicillin. Lyme meningitis, encephalitis, carditis and refractory arthritis may require parenteral therapy, typically ceftriaxone or penicillin. Early recognition and treatment is important to prevent progression to disseminated Lyme disease.
Learning points
Suspect Lyme disease in patients with migratory non-itchy rash resembling multiple forms of erythema migrans.
When suspecting Lyme disease, Western blot testing is the confirmatory test of choice.
Patients with early disseminated cutaneous Lyme disease can be managed outpatient with oral doxycycline.
References
- Shapiro ED. Lyme disease. N Engl J Med. 2014; 370: 1724-1731
- Sanchez E, Vannier E, Wormser GP, Hu LT. Diagnosis, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: A review. JAMA. 2016; 315: 1767-77.