Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Case Report - Open Access, Volume 2
A systematic review of the neglect of non-COVID patients amidst COVID pandemic
Priyanka Mishra*; Amborish Nath; Ajit Kumar; Surbhi Sharma
Department of Anesthesiology and Critical Care, AIIMS Rishikesh, India.
*Corresponding Author: Priyanka Mishra
Department of Anesthesiology and Critical Care, AIIMS
Rishikesh, India.
Email: pmishra15390@gmail.com
Received : Sep 14, 2021
Accepted : Nov 01, 2021
Published : Nov 05, 2021
Archived : www.jcimcr.org
Copyright : © Mishra P (2021).
Abstract
The rapidly evolving health concern for COVID-19 has considerably overshadowed the non-COVID ailments. Ranging from delays in diagnosis and treatment, neglect of mild-moderate diseases resulting into their progression, adverse pregnancy outcomes and many others, an array of the collateral damage of this pandemic is still evolving. We have performed this systematic review about the impact of COVID pandemic on patients suffering from other ailments. Our search was conducted through PubMed, Cochrane and Google scholar databases. We included systematic reviews and meta- analysis, and randomized controlled trials, observational studies, case series and case reports to ensure comprehensiveness of our search. We excluded abstract only articles, news articles, the non-scientific commentaries and reports from the review. Primary outcome was assessment of the impact of COVID pandemic on non-COVID diseases and management strategies for tackling the same. This review showed that this crisis has resulted into a significant delay in routine diagnostic procedures and workup with p value < 0.00001 (OR of 0.36; 95% CI, 0.24 to 0.55). The highest impacts will be seen with preexisting major health priorities like HIV, tuberculosis, malignancy, various non-communicable diseases, reproductive and child health. The chief culprits for this include inadequate supplies of medicines, healthcare staff, diagnostics and other technologies. Expansion of the health care workforce, enhanced health financing and supply chain resilience can help us override this pandemic. Hence, the intersection of COVID-19 with other non- COVID ailments can have drastic effects. To minimize this surplus morbidity and mortality, we need to adopt comprehensive strategies and maintain the momentum even after this pandemic is surpassed.
Keywords: COVID-19; neglect; non-COVID; non-communicable diseases; communicable diseases; management.
Citation: Mishra P, Nath A, Kumar A, Sharma S. A systematic review of the neglect of non-COVID patients amidst COVID pandemic. J Clin Images Med Case Rep. 2021; 2(6): 1398.
Introduction
The global health concern for COVID-19 has considerably overshadowed the non-COVID ailments. These are the patients bearing the brunt as the healthcare systems across the world are attempting to break the crashing tide of COVID pandemic [1]. As of July 14, 2020, WHO has reported 12,964,809 cases of COVID-19 worldwide [2]. The fear and panic associated with the highly contagious nature of coronavirus, coupled with the shifted focus of health care facilities, has culminated into a virtual denial of medical care to a significant portion of the population suffering from other diseases. There has been a raised concern regarding the significant impact of the COVID outbreak on both the emergency response systems and the outpatient services [3]. Ranging from delays in diagnosis and treatment, neglect of mild-moderate diseases resulting in their progression and adverse pregnancy outcomes, the array of the collateral damage of this pandemic is still evolving [4,5].
There is indeed research coming up, describing and quantifying the deleterious impact of COVID-19 on non-COVID patients. However, to the best of our knowledge, no systematic review has yet been done on the toll of COVID outbreak on population having other ailments and the inability to cater to their medical care demands. Our review aims at an evidence-based identification of the various aspects of these negative impacts, lacunas in medical care delivery, and possible optimization of essential health care access to all genres of patients to minimize the collateral damage and enhance patient outcomes.
Objectives
We have done this systematic review to address the critical aspect of neglect of non-COVID patients amidst this pandemic. The main goals behind our review include the due identification of non-COVID morbidity and mortality, probing the evidence associated with the disparity in medical care in them, and identifying the best approaches to minimize the acute and delayed effects on the health of this significant segment of the population. With this review, rather than offering an exhaustive description of the impact on every non-COVID ailment, we aim to contemplate in brief about the specific relevant aspects of this significant health problem, highlight the implication of essential care to all arrays of patients. We also sought to explore the evidencebase on the need for such actions in the current scenario.
Literature search strategy
We performed our initial search between December 2019 to July 2020 to identify published literature on COVID-19 and its impact on non-COVID diseases. All literature was searched for the relevant articles by two researchers independently, and another researcher carefully reviewed the selected abstracts. We conducted a systematic literature search for this review in the online databases of PubMed, Cochrane, and Google scholar. We used a well-formulated PICOS framework to execute this research (Table 1). The combination of keywords that were used for the search included- “COVID-19” AND “non-COVID diseases”, “Coronavirus” AND “communicable diseases”, “COVID-19” AND “non- communicable diseases”, “COVID-19” AND “global health”, “COVID-19” AND “other diseases”, “COVID-19” AND “ pregnancy,” “Coronavirus” AND “Child health”, “COVID-19” AND “mental health”, “COVID-19” AND “Impact” and “COVID-19” AND “Strategies”. We also screened the WHO database of publications on novel coronavirus for any potentially relevant articles. Some publications were also retrieved through crossreferences from published articles.
Table 1: PICOS framework
Interventions |
Diagnosis and Treatment |
||
Controls |
Comparison with patients having confirmed positive coronavirus 2 infection |
||
Outcomes
|
Primary objective-
Secondary objective-
|
||
Study design |
|
Data analysis
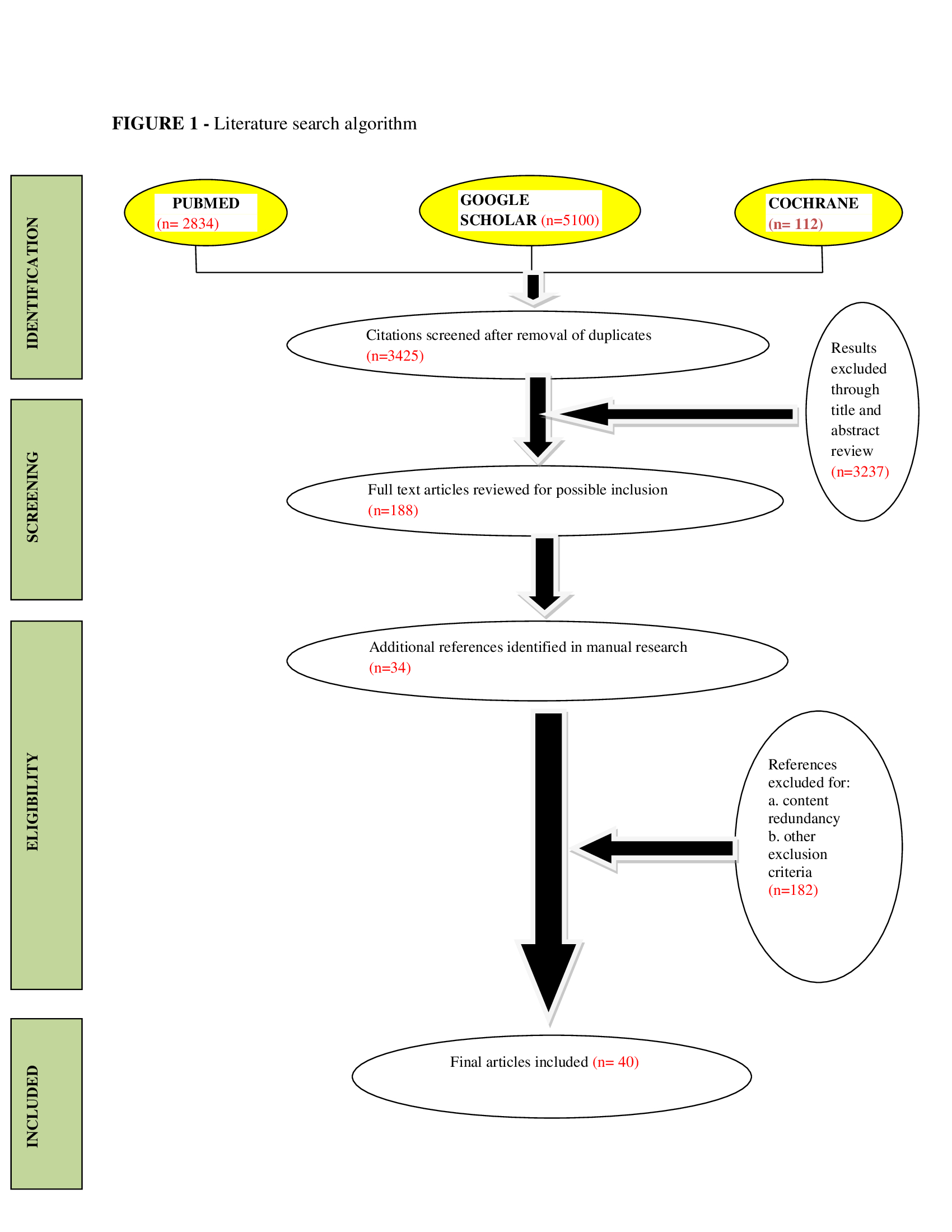
We performed our search giving the highest consideration to systematic reviews and meta-analysis and Randomized Controlled Trials (RCTs), observational studies, case series, and case reports in the decreasing order of consideration. The abstract only articles, news articles, the non-scientific commentaries, and reports were excluded from our analysis. Our initial search showed 8046 articles, from which 40 were finally included in our systematic review. We have conducted this review in compliance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines (Figure 1).
We have incorporated 28 articles documenting clinical studies and systematic reviews conducted in association with the effect of coronavirus infection on other ailments and medical conditions. Guided by the main goals of our research, we have classified these articles into the following research domainsimpact and delay in diagnostics, delay in treatment, disease progression, impact on child morbidity, maternal health, and approaches for improving non-COVID patients outcome.
Delay in diagnostics
As earlier witnessed during the severe acute respiratory syndrome epidemic in 2003, the ambulatory care and inpatient care decreased by 23·9% and 35·2% respectively in Taiwan itself [6]. On a similar trend, the exaggerated focus on tackling COVID affected patients and avoidance of overburdening the health care systems with other general medical care has badly hit the other patients [7,8]. The delay in routine diagnostic procedures as a consequence of this crisis has not only hurt the routine workup but has also delayed the detection of new cases [9]. Low and middle income countries are worst affected as far as the delay in presentation, diagnosis and treatment is concerned. (Figure 2) Filippo et al. reported that there was a significant decrease in acute coronary syndrome (ACS) -related hospitalization rates from 18.0 admissions per day earlier the same year to 13.3 admissions per day during the early days of the Covid-19 outbreak. They also documented a significant increase in mortality during this period that was not fully accountable by Covid-19 cases alone [10].
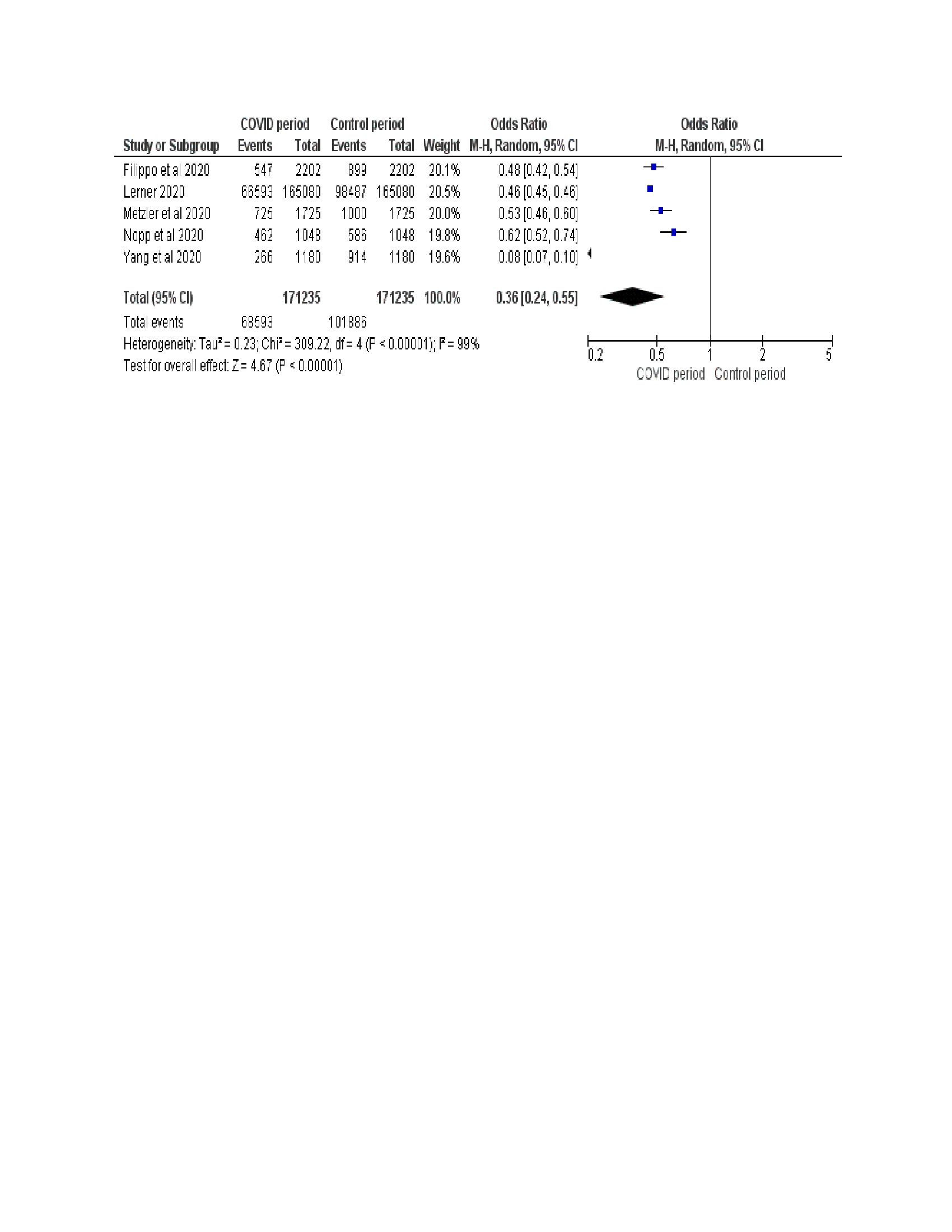
Analysis of studies
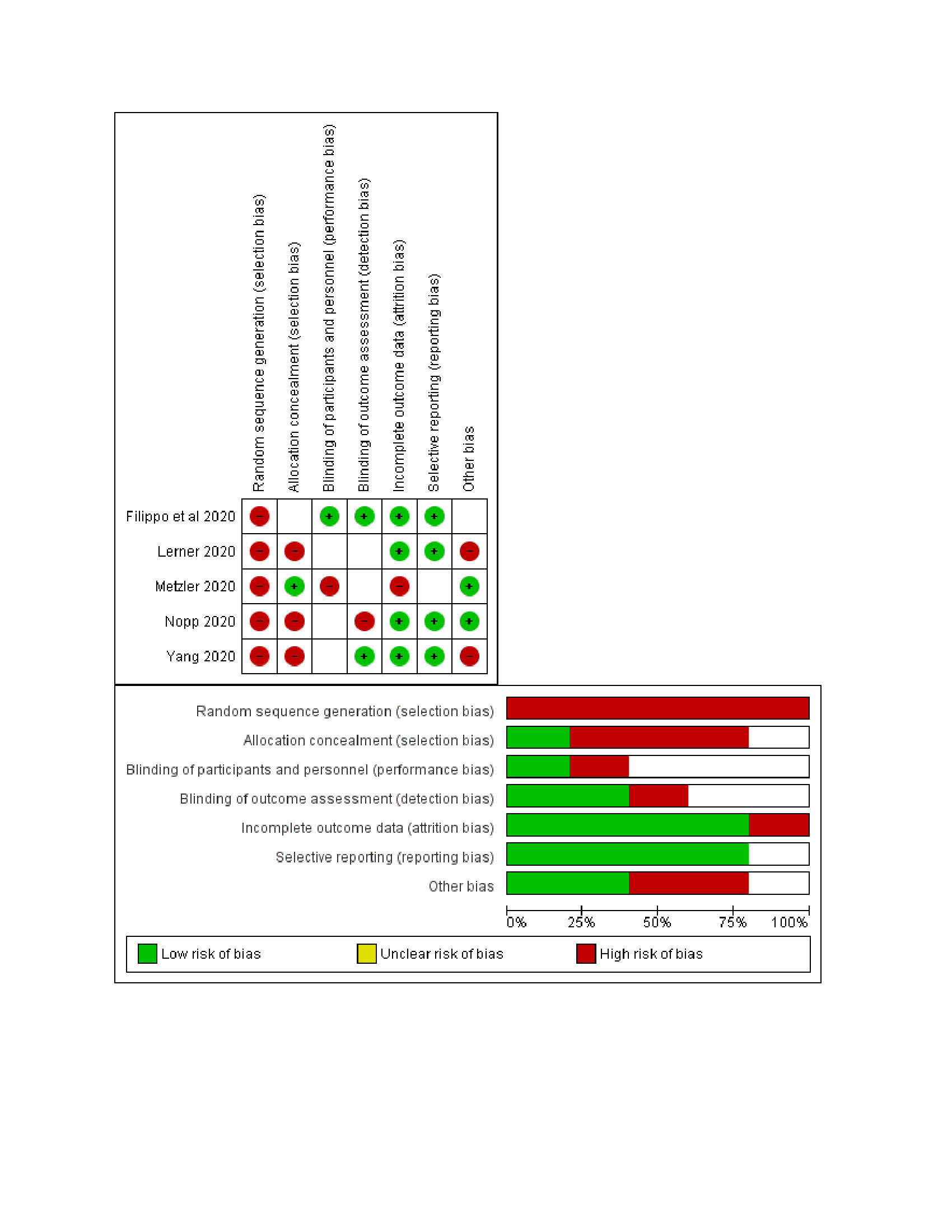
Various other studies have documented a delay in the diagnosis and treatment of non-COVID conditions owing to COVID-19. The comparison of studies evaluating the impact on diagnosis and treatment in non-COVID conditions have been summarized in Table 2. The results revealed that there is a significant decline (OR of 0.36; 95% CI, 0.24 to 0.55) in diagnosis and management of patients presenting with ailments other than COVID-19 with a p value < 0.00001. There is a high heterogeneity found in the study data (I2 =99%). The results are shown in Figure 3. There is an unavoidable selection bias present as all the analysed research is from restrospective observational studies. Few studies suffered from reporting bias owing to multiple entries and lack of complete data reporting.
Table 2: Table of clinical studies on delayed diagnosis and management due to COVID-19.
Study |
Centre, Study design |
Country |
Objectives |
Groups |
n |
Outcomes |
Limitations |
1.Fillipo etal (10) |
multi‐centre,
|
Italy |
Evaluating the rate of hospital admissions for acute coronary syndrome (ACS) during the early Covid-19 outbreak. |
2019 2020 2020 |
756
899
547 |
The mean admission rate for ACS during the lockdown period was 13.3 admissions per day that is significantly lower than either the rate during the earlier period in the same year( 18.0 admissions per day) and in 2019(18.9 admissions per day) |
1.Selection bias |
1.Nopp et al (11)
|
single‐centre, cohort study
|
Austria
|
Changes in the incidence of pulmonary embolism (PE) during COVID‐19 pandemic compared to before the pandemic. |
2018
|
509
|
Compared to weeks 12 to 17 of 2018 and 2019, PE incidence and tests were decreased from 5.3 (95% CI, 3.6‐7.1) to 1.8 (95% CI, 0.0‐3.6) and 31.5 (95% CI, 27.1‐35.9) to 17.3 (95% CI, 11.6‐23.1), respectively. |
1. COVID‐19 patients, who seem to be at high risk for PE, effort was taken to treat them at specific (non-study) hospitals. |
2. Metzler et al(4) |
multi‐centre, |
Austria |
Impact of COVID-19 on the diagnosis and treatment of acute cornary syndrome |
STEMI patients |
354 371
|
Comparing the first and last calendar week, there was a relative reduction of 39.4% in admissions for ACS.
|
|
3. Lerner et al(3)
|
multicentre,
|
United States |
To quantify trends in EMS incidents as the effects of COVID‐19 pandemic.
|
Time 40th to 21st week
2018-19
2019-20 |
8,621,423 13,387,829 15,541,697 |
1.Early in the COVID‐19 outbreak there was a significant decrease by 26.1% between week 10 and week 16 in the number of emergency medical services responses across the United States. |
1.expansion of states participating in NEMSIS during the time frame that was studied. |
4.Yang et al (12)
|
Single centre |
China |
Evaluating |
Before isolation After isolation
|
914 266 |
Significant decline in the median waiting days for pathological biopsy(5 vs 15, P=0.012), radiotherapy immobilization(3.5 vs 16.5, P< 0.001), simulation and initiation of radiotherapy.
|
1.Selection bias. |
Impact on cancer, HIV, and TB
In many countries, the diagnosis and treatment of malignancies are still available only in bigger centres. The course of anti-tumor management, including chemotherapy and radiotherapy, usually runs longer, with several necessary roundtrips between cities. In the current scenario, epidemic control lockdown restrictions on the intercity migration, and hospital admissions may hinder the diagnosis and treatment of cancer patients. It can subsequently result in poor clinical outcomes. A delay in critical interventions and treatment will render earlystage cancers into an advanced inoperable stage [13,14]. Yang et al. found that the number of outpatient visits in the cancer clinic dropped drastically from 914 in 20 weekdays before lockdown to 266 in 20 days after lockdown. On a similar trend, the number of patients who underwent radiotherapy dropped from 52 to 24, respectively [12]. Another study has also confirmed that an increase in the waiting interval for radiotherapy can be detrimental for patient survival [15]. Moreover, various public screening programs, for example, for cervical and breast cancer, have been postponed to curtail non-urgent facility-based services. It is going to result in an unprecedented surprise in cases of advanced-stage malignancies soon.
Particular concern exists in the low and middle-income countries for major health priorities, specifically HIV, tuberculosis, and malaria [16]. As per the analyses from WHO,UNAIDS, and the Stop TB Partnership along with the real-time experiences, the knock-on impact on these three diseases could be even worse than the direct impact of COVID itself [17,18,19]. Hogan et al. concluded that in high-burden situations, mortalities due to HIV, tuberculosis, and malaria over five years could rise by nearly 10%, 20%, and 36%, respectively, with compared to a Non- COVID scenario. The highest impacts on these diseases were estimated owing to the interruption of antiretroviral therapy for HIV (due to diversion for COVID treatment), reductions in diagnosis and treatment of new tuberculosis cases, and interruption of planned net campaigns and hydroxychloroquine supply for malaria [20].
Impact on other communicable diseases
As the coronavirus shares the symptoms of cough, fever, and myalgia with several other viral illnesses, it quickly dominates the differential diagnosis in the current situation [21]. It is resulting in delayed identification and initiation of management of other significantly hazardous conditions like pneumonia, vasculitis, and other viral infections. India alone witnessed more than 4.2 crore cases of acute respiratory infections, 1.3 crores of acute diarrhea, 7.5 lakh cases of pneumonia, 2.2 lakh cases of Typhoid, and one lakh cases of dengue in the year 2017.Wang et al. found in their study that Acute Respiratory Infection (ARI) contributed to 71%, with diarrhea and septicemia, the subsequent most common causes of infant mortality due to communicable diseases [22].
With the governments prioritizing the anti-COVID movement, the rest of the national health programs and missions for the prevention and treatment of various diseases have taken a backfront [23]. It is noteworthy that even the conditions like diarrhea, malaria, and dengue, which are potentially treatable and mostly non-lethal, in the absence of timely interventions, can turn severe and claim many more lives than the COVID 19.
Impact on non-communicable diseases (NCD)
It is noteworthy that the interaction between coronavirus disease 2019 and non-communicable diseases may result in a rise in the global burden of disease. In the year 2017, more than 70% of all deaths globally were accounted for by non-communicable diseases [24]. As per a study conducted over three weeks in 155 countries, which reported interruption of treatment services for hypertension, diabetes and related complications, cardiovascular emergencies, and cancer by 53%, 49%, 31%, and 42%, respectively. The chief culprits for this were inadequate supplies of medicines, healthcare staff, diagnostics, and other technologies [25].
Apart from this, there is evidence suggesting that there might be an association on multiple levels between non-communicable diseases and COVID-19. In high-income countries, many COVID-19-related deaths are older individuals with concurrent NCD [26]. Azarpazhooh et al. found a significant correlation between life expectancy (r = 0.65, p<0.001),non-communicable disease disability-adjusted life years (r = 0.32, p<0.001) and healthy life expectancy (r = 0.63, p<0.001 with COVID-19 cases [27]. It is imperative to understand that presence of non-communicable diseases can also contribute to the risk of developing coronavirus infection. Aggarwal et al. documented a 2.5-fold higher risk of severe COVID-19 disease in patients with a prior history of cerebrovascular illness [28]. Moreover, COVID control measures like physical distancing, quarantine, and lockdown leading to unhealthy dietary habits, physical inactivity, tobacco, and substance use can further result in poor management of NCD.
Impact on pregnancy
Adverse perinatal outcomes have been associated with some viral infections in pregnancy. The immunocompromised state of pregnant females itself increases their vulnerability to acquire coronavirus infection. The transmission through breastfeeding or vertical transmission of the SARS-CoV-2 virus has not been established to date [29]. However, complications like miscarriage, preeclampsia, cesarean section, pre-term birth, and perinatal death have been associated with the coronavirus infection with pneumonia during pregnancy [30]. In addition to the concerns regarding COVID, the delays in regular antenatal visits can potentially affect the routine vaccinations and timely diagnosis of various deleterious conditions. This pandemic has also significantly raised the pre-existing perinatal anxiety and depression. In a cross-sectional study, 46% of women reported high anxiety (as VAS for anxiety score ≥50), concerning the vertical transmission of the virus and disease [31]. It is expected that with a rise in unwanted pregnancies and reduced access to medical abortion drugs, reproductive health is going to suffer badly.
Child morbidity and mortality
It is predicted that owing to the seismic shift in health care priorities created by this pandemic; it is also going to impact the access to food and healthcare among children [32]. It can be further assumed that this impact is going to be more drastic in low and middle-income countries. As mentioned earlier in the text, the prime challenges in the pursuit of their care will include – a) delayed recognition and referral for various malignancies and other disorders; b) disruption in the supply chain of essential drugs; c) reduced blood products supply due to shortage of donors; d) enhanced psychosocial strains on families dealing with already sick children; e) families living at or below poverty lines, losing their incomes and capacities to support even the basic needs. Without proper address to these challenges, the child morbidity and mortality could take overwhelming numbers, even in those otherwise having a low risk of mortality due to the coronavirus itself [33].
Risks to mental health
COVID-19 is not only going to affect physical health but will also cast a significant negative impact on both acute and longterm mental health. As the nonemergency medical care is being restricted or unavailable for a multitude of other distressing and troublesome conditions, the collateral damage will become overwhelming. The stress of job insecurity, financial losses, forced lifestyle modifications, including lack of alcohol and other substances of abuse, can serve as potential triggers for anxiety and other depressive disorders [34]. The effects of this stress can be delayed, and the risks of mental infirmity may linger high for years, and even decades after the passage of stress [35].
There is an elevated risk of worsening and relapse in patients with existing mental illness in the advent of the inability to access medicines or consultations due to lockdown. Also, there can be a rush of new cases of both major and minor mental illnesses in the months and years to come. Aranda et al. found in their study that there was worsening in patients with prepandemic eating disorders and anxiety by 37.5% and 56.2% after the outbreak of COVID-19 [36]. Various studies have reported a significant rise in psychological distress and symptoms like depression, anxiety, sleep disorders among the health care workers due to the current global health crisis [37-39].
This imminent fear, bordering on panic, can also contribute to a rise in suicidal tendencies among people. There can be a high risk of post-traumatic stress disorder in patients kept in isolation or quarantine [40].
Strategies for management
It is imperative to acknowledge that to prevent denial of health services to any proportion of the population, we need to set up dedicated Covid-19 facilities while allowing remaining medical facilities to continue to cater to other non-COVID healthcare services. The dooming effect of various non-COVID communicable and non – communicable diseases can be minimized by the maintenance of core services and providing continuous access to essential medicines. In the times of this global health crisis, it is essential to create and sustain the sense of confidence in the health care system amongst the general population. The Reproductive, maternal, newborn, and child health services (like essential child immunizations) should be prevented from coming to a halt. While the pandemic is still evolving, statistical modeling of specific, quantifiable estimates is required to have a reference point for policymakers.
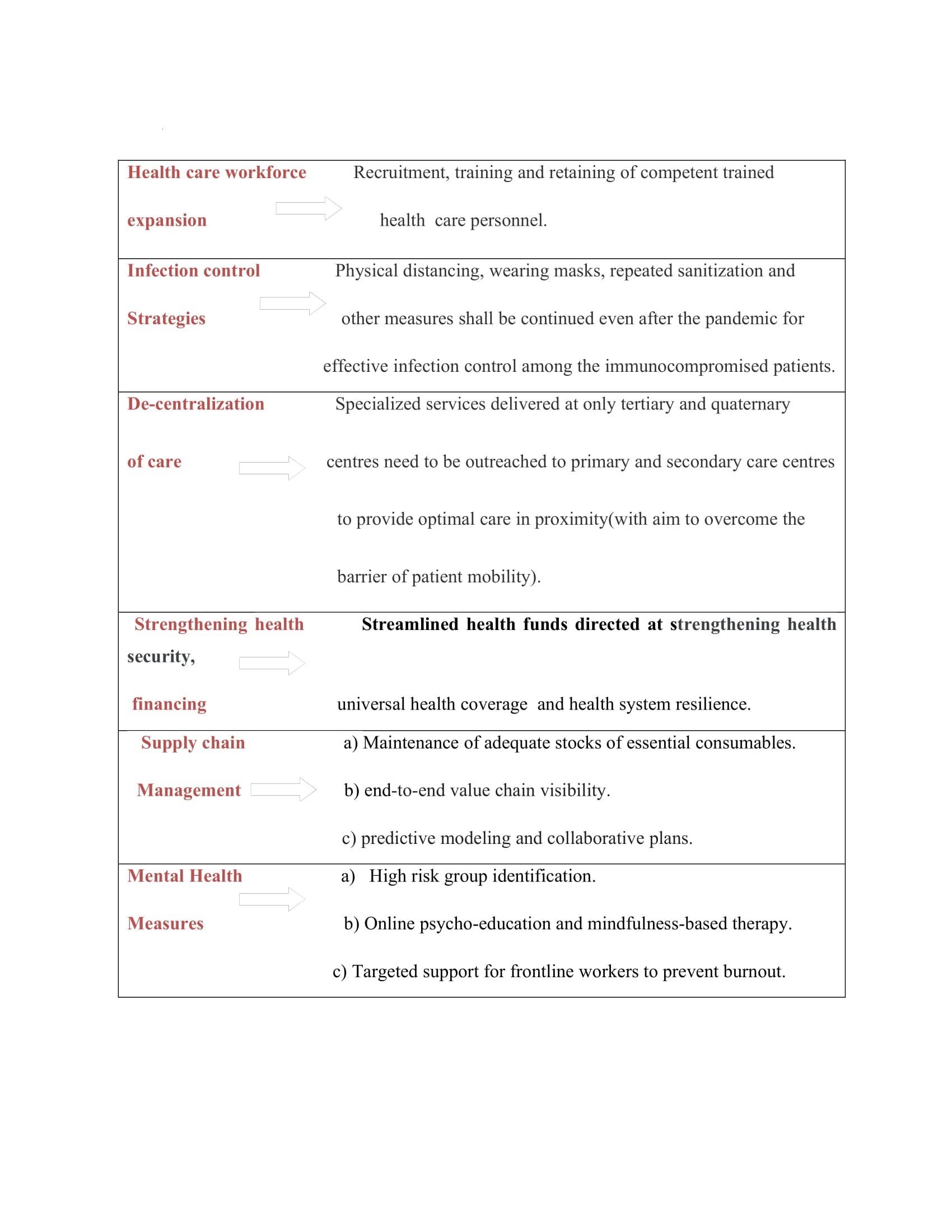
Expansion and strengthening of the health care workforce will not only help us tide the pandemic but can be re-allocated later to cater to the multitude of communicable and non-communicable diseases (Figure 5).
Telemedicine is offering a healthy alternative to replace inperson consultations. However, it has its limitations as it cannot provide for a proper clinical examination and evaluation, which is the key to an accurate diagnosis. Hence, there is a need for the long term and holistic approaches to achieve a sustainable health system. We should recognize this wake-up call and continue the momentum formed in response to the COVID pandemic to harness positive implications for health care systems in times to come.
Strengths
Although, there are systematic reviews on the impact of COVD-19 pandemic on mental health, maternal and child health outcomes individually, this is the first systematic review, to the best of our knowledge that summarizes the current evidence on the impact of COVID-19 pandemic on all other non-COVID diseases.
Limitations
We completely acknowledge the most significant limitation of our research is the brief period of seven months over which the search was conducted. The second limitation exists in the form of an unavoidable inherent bias, which could be in terms of patient selection, lockdown and treatment protocols. An unavoidable selection bias exists due to the heterogeneity in terms of types of studies as we have included data from observational studies, case series, or case reports. Another limitation includes the probable multiple comorbidities in some patients, which can produce an added effect on critical events.
Conclusion
It is essential to understand the intersection of COVID-19 with other non- COVID ailments and planning appropriate strategies to avoid the untoward effects of the same. The virtual defiance of health care services to all those suffering from other conditions will add to both the morbidity and mortality in current times and the times to come. We need to sustain the momentum acquired against this pandemic to efficiently tackle the more significant struggles once we override the tide of COVID-19.
References
- Rosenbaum L. The Untold Toll — The Pandemic’s Effects on Patients without Covid‐19. New England Journal of Medicine. 2020.
- Organization H W. WHO Coronavirus Disease (COVID-19) Dashboard. 2020.
- Lerner BE, Newgard DC, Mann CN. Effect of the Coronavirus Disease 2019 (COVID-19) Pandemic on the U.S. Emergency Medical Services System: A Preliminary Report.Academic Emergency Medicine. 2020; 00: 1– 7.
- Metzler B, Siostrzonek P, Binder RK, Bauer A, Reinstadler SJ. Decline of acute coronary syndrome admissions in Austria since the outbreak of COVID-19: the pandemic response causes cardiac collateral damage. Eur Heart J. 2020; 41: 1852– 3.
- Mascio DD, Khalil A, Saccone G, Rizzo G, Buca D, Liberati M, et al. Outcome of Coronavirus spectrum infections (SARS, MERS, COVID 1 -19) during pregnancy: A systematic review and metaanalysis. Am J Obstet Gynecol MFM. 2020; 100-07.
- Chang HJ, Huang N, Lee CH, Hsu YJ, Hsieh CJ, Chou YJ. The impact of the SARS epidemic on the utilization of medical services: SARS and the fear of SARS. Am J Public Health. 2004; 94: 562–64.
- Saglietto A, D’Ascenzo F, Zoccai GB, De Ferrari GM. COVID-19 in Europe: The Italian lesson. Lancet. 2020; 395: 1110-1.
- Grasselli G, Pesenti A, Cecconi M. Critical care utilization for the COVID-19 outbreak in Lombardy, Italy: early experience and forecast during an emergency response. JAMA. 2020.
- Tam C‐CF, Cheung K‐S, Lam S, Wong A, Yung A, Sze M, et al. Impact of Coronavirus Disease 2019 (COVID-19) Outbreak on ST‐Segment‐Elevation Myocardial Infarction Care in Hong Kong. China. Circulation: Cardiovascular Quality and Outcomes. 2020; 13: e006631.
- De Filippo O, D’Ascenzo F, Angelini F, Bocchino PP, Conrotto F, Saglietto A, et al. Reduced rate of hospital admissions for ACS during Covid-19 outbreak in Northern Italy. N Engl J Med. 2020.
- Nopp S, Janata-Schwatczek K, Prosch H, et al. Pulmonary embolism during the COVID-19 pandemic: Decline in diagnostic procedures and incidence at a university hospital. Res Pract Thromb Haemost. 2020; 4: 835-841.
- Yang Y, Shen C, Hu C. Effect of COVID-19 Epidemic on Delay of Diagnosis and Treatment Path for Patients with Nasopharyngeal Carcinoma. Cancer Manag Res. 2020; 12: 3859-3864.
- Stoker SD, Wildeman MA, Fles R, et al. A prospective study: current problems in radiotherapy for nasopharyngeal carcinoma in yogyakarta, indonesia. PLoS One. 2014; 9: e85959.
- Liang H, Xiang YQ, Lv X, et al. Survival impact of waiting time for radical radiotherapy in nasopharyngeal carcinoma: A large institution-based cohort study from an endemic area. Eur J Cancer. 2017; 73: 48–60.
- Chen YP, Mao YP, Zhang WN, et al. Prognostic value of wait time in nasopharyngeal carcinoma treated with intensity modulated radiotherapy: A propensity matched analysis. Oncotarget. 2016; 7: 14973–14982.
- Walker PGT, Whittaker C, Watson OJ et al. The impact of COVID-19 and strategies for Mitigation and suppression in low- and middle-income countries. Science. 2020.
- Organization H W. The potential impact of health service disruptions on the burden of malaria. 2020.
- Organization H W. The cost of inaction: COVID-19-related service disruptions could cause hundreds of thousands of extra deaths from HIV. 2020.
- Stop TB Partnership. The devastating effect of the COVID-19 pandemic on the TB response: a minimum of 5 years of progress lost and 6 million additional people ill with TB. 2020.
- Hogan AB, Jewell BL, Sherrard-Smith E et al. Potential impact of the COVID-19 pandemic on HIV, tuberculosis, and malaria in low-income and middle-income countries: A modelling study. Lancet Glob Health. 2020.
- A.J. Rodriguez-Morales, J.A. Cardona-Ospina, E. GutierrezOcampo, et al. Clinical, laboratory and imaging features of COVID-19: A systematic review and meta-analysis. Travel Med Infect Dis. 2020; 34: 101623.
- Wang K, Xiang L, Kang L. et al. Communicable disease mortality trends and characteristics of infants in rural China, 1996–2015. BMC Public Health. 2020; 20: 455.
- Gopalan HS, Misra A. COVID-19 pandemic and challenges for socio-economic issues, healthcare and National Health Programs in India [published online ahead of print, 2020 May 30]. Diabetes Metab Syndr. 2020; 14: 757-759.
- Martinez R, Lloyd-Sherlock P, Soliz P. Trends in premature avertable mortality from non-communicable diseases for 195 countries and territories, 1990-2017: a population-based study. Lancet Glob Health. 2020; 8: e511–e523.
- Organization HW. COVID-19 significantly impacts health services for non-communicable diseases. 2020.
- McMichael TM, Currie DW, Clark S. Epidemiology of COVID-19 in a long-term care facility in King county, Washington. N Engl J Med. 2020; 382: 2005–2011.
- Azarpazhooh MR, Morovatdar N, Avan A, et al. COVID-19 Pandemic and Burden of Non-Communicable Diseases: An Ecological Study on Data of 185 Countries. J Stroke Cerebrovasc Dis. 2020; 29: 105089.
- Aggarwal G, Lippi G, Michael Henry B. Cerebrovascular disease is associated with an increased disease severity in patients with Coronavirus Disease 2019 (COVID-19): A pooled analysis of published literature. Int J Stroke. 2020; 15: 385-389.
- Yan J, Guo J, Fan C, et al. Coronavirus disease 2019 in pregnant women: a report based on 116 cases. Am J Obstet Gynecol 2020; 223: 111.e1-14.
- Di Mascio D, Khalil A, Saccone G, Rizzo G, Buca D, Liberati M, et al. Outcome of Coronavirus spectrum infections (SARS, MERS, COVID 1 -19) during pregnancy: A systematic review and metaanalysis. Am J Obstet Gynecol MFM. 2020; p. 100107.
- Saccone G, Florio A, Aiello F, et al. Psychological impact of coronavirus disease 2019 in pregnant women. Am J Obstet Gynecol. 2020; S0002-9378(20)30527-5.
- Roberton T, Carter ED, Chou VB, et al. Early estimates of the indirect effects of the COVID-19 pandemic on maternal and child mortality in low-income and middle-income countries: a modelling study. Lancet Global Health. 2020.
- Dong Y, Mo X, Hu Y, et al. Epidemiology of COVID-19 among children in China. Pediatrics. 2020.