Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Case Report - Open Access, Volume 3
Ultrasound-guided intervention for chronic abdominal wall pain; Overlooked but curative approach
Farzan Vahedifard1*; Gholamreza Raissi2; Tannaz Ahadi3; Bijan Forogh2 ; Ali Afrasiabi4
1 Neuromusculoskeletal Research Center, Department of Physical Medicine and Rehabilitation, School of Medicine, Iran University of Medical Sciences, Tehran, Iran.
2 Professor, Neuromusculoskeletal Research Center, Department of Physical Medicine and Rehabilitation, School of Medicine, Iran University of Medical Sciences, Tehran, Iran.
3 Associate Professor Neuromusculoskeletal Research Center, Department of Physical Medicine and Rehabilitation, School of Medicine, Iran University of Medical Sciences, Tehran, Iran.
4 General Physician, Iran University of medical science, Tehran, Iran.
*Corresponding Author: Farzan Vahedifard
Neuromusculoskeletal Research Center, Department of Physical Medicine and Rehabilitation,
School of Medicine, Iran University of Medical Sciences, Tehran, Iran.
Email: Farzanvahedi@yahoo.com
Received : Apr 11, 2022
Accepted : May 09, 2022
Published : May 16, 2022
Archived : www.jcimcr.org
Copyright : © Vahedifard F (2022).
Abstract
One of the most common causes of chronic abdominal pain is ‘Chronic Abdominal Wall Pain, “CAWP”, which frequently goes undiagnosed. CAWP accounts for 10-30% of patients in surgical, gynecological, and gastrointestinal clinics who have a primary complaint of persistent abdominal pain. CAWP, on the other hand, may be treated quickly and efficiently using a neuro intervention approach. This study provides a real-world example of a 40-year-old man who has CAWP in the right bottom quadrant. Endoscopic, imaging and biochemical results were all normal. With a positive Carnett’s sign and probable CAWP, she was given an ultrasound-guided injection of 2 percent lidocaine in the suspected nerve entrapment location, with no recurrence discomfort. Significant CAWP management include reassurance, activity moderation, physical therapy, and pain control. Local anesthetic and steroid injection can be used for both diagnostic and curative purposes. There is an evident lack of knowledge regarding the diagnosis and treatment of AWPs among physicians. However, a sensitive and straightforward finding (Carnett’s Sign) in the physical examination can help quickly diagnose AWPs which in turn, in many cases, can be treated effectively.
Keywords: CAWP; Abdominal wall pain.
Citation: Vahedifard F, Raissi G, Ahadi T, Forogh, Afrasiabi A. Ultrasound-guided intervention for chronic abdominal wall pain; Overlooked but curative approach. J Clin Images Med Case Rep. 2022; 3(5): 1836.
What is CAWP
Either organic or non-organic causes can cause chronic abdominal pain. Organic non-visceral causes are related with abdominal wall structures, including muscles, fascia, and nerves [8]. Chronic abdominal wall pain (CAWP) is described as chronic or intermittent pain in the abdominal area that lasts at least three to six months [1]. A dramatic drop in the patient’s quality of life and negative personal and work-related consequences raises healthcare expenses, superfluous diagnostic testing, and treatments for visceral diagnoses [2]. The following are the characteristics of abdominal discomfort that originates in the abdominal wall:
The pain is typically constant or intermittent and is seldom paroxysmal. The intensity of pain is dependent on the patient’s posture and is exacerbated by physical activity (such as exercise, coughing, or sneezing). Pain has no bearing on digestion or intestinal function. When the abdominal wall is stretched, abdominal soreness increases dramatically. The trigger points are often smaller than 2 cm in diameter. The trigger point is frequently located on the lateral edge of the rectus abdominal muscle or is related to the abdominal muscle or fascia. By stimulating the trigger point, the pain is extended to a larger region [3,4].
Physical examination of CAWP
Physical examination of the abdomen enables the physician to differentiate relatively well between visceral and non-visceral pain. Contraction of the abdominal wall and simultaneous elevation of the head and shoulders from the bed in the supine position, lessens the pain with an intra-abdominal origin. In contrast, the pain with abdominal wall origin stays the same or worsens (referred to as a positive Carnet Sign). Carnett was a surgeon who described the clinical features of CAWP [5]. The patient sleeps in a supine position for examination. Most patients localize the pain site precisely by fingertips (Trigger Point). Usually, its margin has a maximum of 2 cm in diameter and is on the semilunar line (the outer margin of the rectus abdominal muscle). Since the pain is localized, the patient is urged to contract his abdominal wall, either by lifting his extended foot or by raising the upper half of his body without using his arms. When the abdominal muscles are tightened, pressing with a single finger on the most painful region frequently exacerbates the pain (positive Carnett’s sign). However, aggravation may not occur in the absence of tightness. By contrast, people with abdominal visceral discomfort get alleviation when their abdominal muscles are contracted (negative Carnett’s sign) [6]. To conduct the test successfully, adequate cooperation and voluntary contraction of the anterior abdominal muscles are required.
Available treatment for CAWP
Reassurance, activity modification, physical therapy, and pain management are key CAWP therapies. Patient education is critical in therapy. Pain alleviation from a local anesthetic injection frequently helps persuade the patient.
There are four treatments: 1- Local anesthetic injection 2- Local anesthesia and steroid injection 3- Phenol neurolysis 4- Nurectomy or nerve decompression [7]
Maybe some other neuro-intervention that can be used in the future for the treatment of peripheral neuropathies may be future indications of neuro-intervention and neuromodulation [8].
Real case management
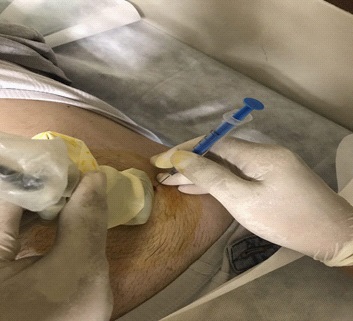
This study provides a real-world example in our physical medicine and rehabilitation clinic. A 40-year-old man with CAWP in the right lower quadrant for the past one year, refer to our clinic. His pain started suddenly without any stimuli and increased in times of stress but without any associated symptoms. The severity of the pain has not been to prevent the patient from daily work. Endoscopic and imaging were normal. The patient’s biochemistry was normal. Given a positive Carnett’s sign and suspected CAWP, she was given an ultrasound-guided injection in nerve entrapment suspected area with 2% lidocaine, with no recurrent pain (Figure 2).
Discussion and conclusion
CAWP is one of the challenges that primary care physicians and specialists face. Previous research has found that only approximately 1% of patients and clinicians are aware of AWP as a cause of CAWP. Only 4% of clinicians that visited CWAP used AWP as their initial diagnosis [4]. For many years, individuals with CAWP were exposed to endoscopy, colonoscopy, diagnostic laparoscopy, laparotomy, and a range of imaging and laboratory testing and other diagnoses such as IBS and chronic pancreatitis. Patients will eventually be unsatisfied with the outcome of their treatment. If simple physical tests and a comprehensive history test (as described in the checklist elements) can be used to discover the cause of AWP. Furthermore, medical professionals (including gastroenterologists, gastrointestinal surgeons, urologists, and gynecologists) believe that CAWP is caused only by visceral disorders. All of this suggests that doctors are unfamiliar with the etiology of AWP [9].
However, the abdominal wall is the source of pain in 10% to 90% of patients with unclear abdominal pain, or 10% of all abdominal pain patients referred to gastrointestinal clinics. It is worth mentioning that few researchers have addressed this issue from the standpoint of PM & R, although many AWPs are treated with various PM & R modalities. Local anesthetic injections, for example, can reduce pain in 60 to 90 percent of patients and confirm the diagnosis [10]. CAWP is a prevalent clinical disease [11] CAWP was found in 20% of patients hospitalized to surgery for abdominal discomfort [15]. In the Srinivasan research, 10–90% of individuals with unclear etiology stomach discomfort had AWP [9].
Neuroradiology and ultrasound can be used in various situations, such as when a diagnosis is uncertain or a patient is not ready for intervention [18,19]. A nerve conduction test is a gold standard for some peripheral neuropathies (CTS). When CTS causes discomfort in a patient, we can replace it with ultrasonography. For example, according to the Mirzasgari et al. study, US can be used as a reliable diagnostic biomarker for diagnosing carpal tunnel syndrome as a common peripheral neuropathy [12]. Anterior cutaneous nerve entrapment (ACNES) was identified as the major cause of AWP by Asan et al. in 2013. This study created an 18-question checklist. ACNES detection had 92% specificity and 94% specificity when 10 of the 18 ACNES checklist questions were positive [13].
While ACNES is not known to induce CAWP in adults, it is a prominent source of abdominal pain in children. ACNES, like CAWP, can lead a kid to be sent to a psychiatrist. Three cases of ACNES were studied and treated with a nerve block [14]. CAWP therapy is based on local trigger point injections. A retrospective study of 110 individuals with abdominal pain who had local trigger point injections found that 89 of them experienced CAWP. After a median of 25 months of Using topical injections to diagnose and treat CAWP, 77% of patients had full remission, however, 23% reported no relief in their symptoms. A good reaction to trigger point injection was predicted by CAWP criteria, absence of gastrointestinal symptoms, and localization of discomfort in the upper abdomen region [15].
In this regard, Alnahhas has investigated using a steroid, a local anesthetic, or a combination of both in ultrasound-guided trigger point injections [16]. According to their findings, the most common site of CAWP was the right upper quadrant, and the median pain duration was 12 months. On the TEQ, 44 of the 120 patients (37 percent) matched the criterion for the responder. In comparison to before therapy, 36% said they were “much better” and 22% said they were “somewhat better.” Higher somatization indicated a worse reaction. There was no correlation between the reaction to the TPI and any of the other history, examination, or TPI features. They claimed that TPI can provide considerable, long-term symptom alleviation in a third of individuals with persistent abdominal discomfort caused by CAWP. Treatment success was inversely associated to somatization. Other neuro-intevention can be combined by neuroimaging and used with nerves or target organs in any location. Different pain-producing components, for example, can be ablated or manipulated by radiofrequency to reduce pain under the guidance of imaging [17].
Suggestion
Well-trained physicians, particularly neurologists, physiatrists, and surgeons, can relieve a great deal of the chronic abdominal pain patients’ helplessness by considering a possible diagnosis of CAWP, performing a simple physical examination, and then ordering neuro intervention modalities such as physiotherapy, manipulation, and nerve block that can be performed even in the office setting.
References
- Spee LA, Lisman-Van Leeuwen Y, Benninga MA, Bierma-Zeinstra SM, Berger MY. Prevalence, characteristics, and management of childhood functional abdominal pain in general practice. Scandinavian journal of primary health care. 2013; 31(4): 197-202.
- Chiou E, Nurko S. Management of functional abdominal pain and irritable bowel syndrome in children and adolescents. Expert review of gastroenterology & hepatology. 2010; 4(3): 293- 304.
- Suleiman S, Johnston DE. The abdominal wall: an overlooked source of pain. American family physician. 2001; 64(3): 431-8.
- Costanza CD, Longstreth GF, Liu AL. Chronic abdominal wall pain: clinical features, health care costs, and long-term outcome. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association. 2004; 2(5): 395-9.
- Takada T, Ikusaka M, Ohira Y, Noda K, Tsukamoto T. Diagnostic usefulness of Carnett’s test in psychogenic abdominal pain. Internal medicine (Tokyo, Japan). 2011; 50(3): 213-7.
- Kamboj AK, Hoversten P, Oxentenko AS. Chronic Abdominal Wall Pain: A Common Yet Overlooked Etiology of Chronic Abdominal Pain. Mayo Clinic proceedings. 2019; 94(1): 139-44.
- Koop H, Koprdova S, Schürmann C. Chronic Abdominal Wall Pain: A Poorly Recognized Clinical Problem. Dtsch Arztebl International. 2016;113(4):51-7.
- Vahedifard F, Malinowski M, Chakravarthy K. Mechanism of Action of Radiofrequency Ablation. In: Deer TR, Azeem N, editors. Essentials of Radiofrequency Ablation of the Spine and Joints. Cham: Springer International Publishing. 2021; 7-29.
- Srinivasan R, Greenbaum DS. Chronic abdominal wall pain: a frequently overlooked problem. Practical approach to diagnosis and management. The American journal of gastroenterology. 2002; 97(4): 824-30.
- Spiegel BM, Farid M, Esrailian E, Talley J, Chang L. Is irritable bowel syndrome a diagnosis of exclusion?: a survey of primary care providers, gastroenterologists, and IBS experts. The American journal of gastroenterology. 2010; 105(4): 848-58.
- Lara FJP, Berges AF, Quesada JQ, Ramiro JAM, Toledo RB, Muñoz HO. Thoracic Disk Herniation, a not Infrequent Cause of Chronic Abdominal Pain. International Surgery. 2012; 97(1): 27-33.
- Mirzaasgari Z, Haghi-Ashtiani B, Refaiean F, Vahedifard F, Homayooni AS, Sobhkhiz M. Diagnostic value of high-frequency ultrasound in carpal tunnel syndrome during pregnancy: A casecontrol study: Tehran University of Medical Sciences; 2021; 73- 7.
- van Assen T, de Jager-Kievit JW, Scheltinga MR, Roumen RM. Chronic abdominal wall pain misdiagnosed as functional abdominal pain. Journal of the American Board of Family Medicine: JABFM. 2013; 26(6): 738-44.
- Akhnikh S, de Korte N, de Winter P. Anterior cutaneous nerve entrapment syndrome (ACNES): the forgotten diagnosis. European journal of pediatrics. 2014; 173(4): 445-9.
- Nazareno J, Ponich T, Gregor J. Long-term follow-up of trigger point injections for abdominal wall pain. Canadian journal of gastroenterology = Journal canadien de gastroenterologie. 2005;19(9):561-5.
- Alnahhas MF, Oxentenko SC, Locke GR, 3rd, Hansel S, Schleck CD, Zinsmeister AR, et al. Outcomes of Ultrasound-Guided Trigger Point Injection for Abdominal Wall Pain. Digestive diseases and sciences. 2016; 61(2): 572-7.
- Chakravarthy K, Golovac S, Vahedifard F. Future Indications. Essentials of Radiofrequency Ablation of the Spine and Joints: Springer. 2021; 241-81.
- Cheung H, Yechoor A, Behnia F, Abadi AB, Khodarahmi I, Soltanolkotabi M, et al. Common Skeletal Neoplasms and Nonneoplastic Lesions at 18F-FDG PET/CT. Radio Graphics. 2021; 42(1): 250-67’
- Haseli S, Mansoori B, Shafiei M, Shomal Zadeh F, Chalian H, Khoshpouri P, et al. A Review of Posteromedial Lesions of the Chest Wall: What Should a Chest Radiologist Know? Diagnostics. 2022; 12(2): 301.