Journal of Clinical Images and Medical Case Reports
ISSN 2766-7820
Clinical Image - Open Access, Volume 3
Oesophageal haemangioma
Rabia Azam; Husein Kaderbhai*; Hafsa Zafar; Fahad Rathore; Joseph Mullineux; Sudarshan Kadri
University Hospitals of Leicester NHS Trust, UK.
*Corresponding Author: Husein Kaderbhai
University Hospitals of Leicester NHS Trust, UK.
Email: h.kaderbhai@doctors.org.uk
Received : May 09, 2022
Accepted : May 23, 2022
Published : May 30, 2022
Archived : www.jcimcr.org
Copyright : © Kaderbhai H (2022).
Citation: Azam R, Kaderbhai H, Zafar H, Rathore F, Mullineux J, et al. Oesophageal haemangioma. J Clin Images Med Case Rep. 2022; 3(5): 1860.
Case description
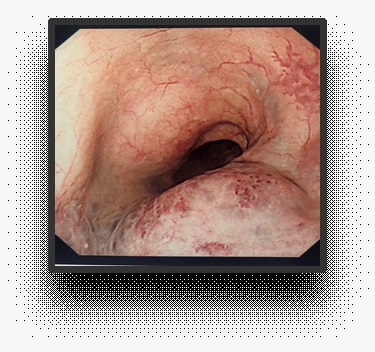
A 76 year old male presented with a few months history of weight loss, abdominal pain, altered bowel habits and dyspepsia despite being on lansoprazole. He was referred for a Gastroscopy (OGD) under the 2 week wait cancer pathway. OGD showed a smooth pigmented mucosal lesion in the mid oesophagus of unknown aetiology. Laboratory investigations were unremarkable.
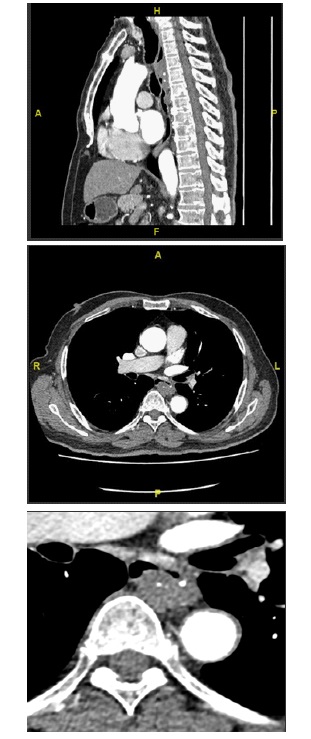
The patient subsequently had a Computerized Tomography (CT) scan which showed a long segment (approximately 8 cm) oesophageal lesion predominantly in the posterior and left lateral aspects, measuring 22 x 14 mm on axial dimensions. There were diffuse calcific foci within the lesion in keeping with phleboliths. No appreciable hyper-enhancement was noted on the arterial phase of the study. This appearance on CT scan was consistent with oesophageal haemangioma.
This case was discussed in upper GI MDT and it was decided to continue with conservative management as the patient did not have any dysphagia or previous history of hematemesis.
Oesophageal haemangiomata are rare benign vascular tumours accounting for 3% of benign tumours. Though they are rare, they can usually be identified by specific imaging features aided with clinical symptoms and endoscopic findings, instead of biopsy. It is important to consider this diagnosis as a oesophageal haemangioma can mimic malignancy and can lead to fatal complications including severe haemorrhage if biopsied. This case highlighted typical radiological features of a oesophageal haemangioma which aided us in correct diagnosis without the need of an invasive biopsy.